Lessons from health insurance responses in counteracting COVID-19: a qualitative comparative analysis of South Korea and three influential countries | Archives of Public Health

COVID-19 wave and timeline of health insurance response
Prior to comparing the financial support policies regarding the COVID-19 pandemic, the current COVID-19 status of each country was examined (Fig. 2). The four countries shared a similar pattern in which the first confirmed case of COVID-19 was reported in January 2020 and increases in confirmed case numbers occurred around March to April. Subsequently, a slight decrease was observed in case numbers until the case numbers increased once again at various times in the three countries, excluding Germany (Korea – September, Japan – August, United States – July–August). In November, another wave in confirmed case numbers was observed.
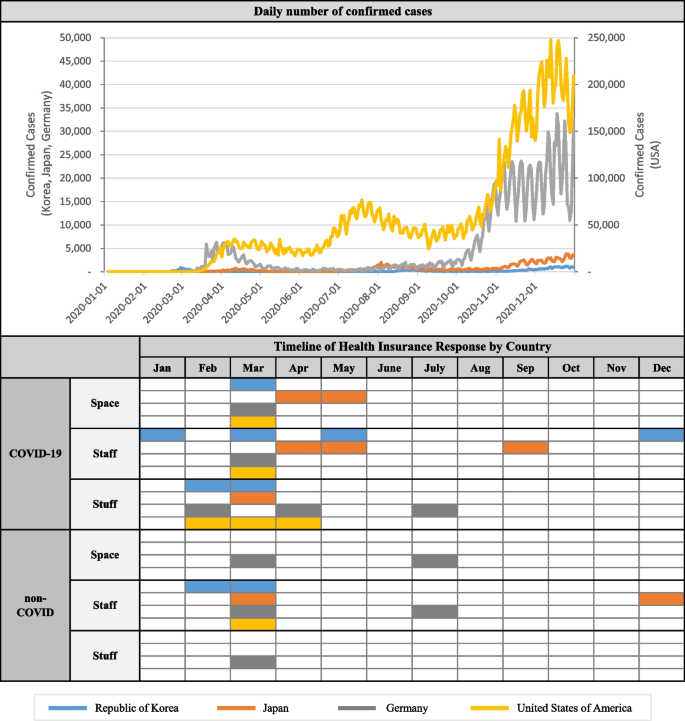
Timeline of Policy Implementation by Country
Examining the pattern of COVID-19 outbreaks and the timing of health insurance intervention implementation reveals that a comprehensive policy implementation of space, staff, and stuff occurred for both the “COVID-19” and “non-COVID” domains in March and April, when the confirmed case numbers rapidly increased.
All four countries implemented simultaneous health insurance policy interventions during the first wave, indicating that social health insurance initiated a response from the early stages of the COVID-19 spread. Therefore, the timing of health insurance system intervention during this major crisis affecting the healthcare systems, namely, the first wave of COVID-19, seemed to be minimally influenced by factors such as the composition of private providers, population coverage, and characteristics of the reimbursement systems.
Among the systems, the implementation of staff was quickest in Korea’s COVID-19 response, as were its responses in the “non-COVID” domain. The single-payer and fee-for-service (FFS) framework of Korea’s incentive system facilitated a relatively smooth increase in testing capacity by healthcare professionals within a short period.
Even after the initial policy intervention, continuous policy intervention efforts, including the supplementation of existing interventions or implementation of additional policies, were observed regardless of the increase pattern of confirmed cases. This trend appeared consistent across all countries, irrespective of the characteristics of their respective health systems. However, the United States concentrated its main support efforts in the COVID-19 domain, with the timing of its interventions tending to align with the first wave. Its degree of health insurance intervention might have been lower than that in the other countries because its Medicare covers a limited population compared with the national insurance in the other countries.
Health insurance response according to analytical framework
We compared the detailed response domains and health insurance implementation targeting COVID-19 and non-COVID patients in each country based on our analytical framework (Table 2). Generally, the COVID-19 domain commonly involved additional compensation to address costs related to providing inpatient services for confirmed patients. Given the need for inpatient treatment for highly contagious confirmed COVID-19 patients using negative pressure wards to prevent transmission to other patients, costs pertaining to such services were made eligible to claim. The space sub-domain involved compensation for the hospitalization fees of COVID-19 patients—the most basic of inpatient service costs. In both Korea and the United States, the hospitalization fees for confirmed patients were increased by 20% compared to the existing level of compensation for inpatient care fees [9, 48]. In Japan, an additional fee for inpatient care for type-2 infectious disease is charged from patients with an infectious disease to account for the increase (up to four times) in infection risk [49]. In the United States, hospitalization fees were increased in accordance with the Coronavirus Aid, Relief, and Economic Security Act (hereafter CARES Act), applied retroactively from January 27, before the enforcement date.
As the compensation of hospitalization fees in the United States was based on the diagnosis-related group (hereafter DRG), the increase in fees offered comprehensive support for not only space but also staff and stuff. The hospitalization fees for intensive care units (ICUs) were increased by 6% in Korea [9] while, in Japan, two revisions led to a fourfold increase in fees [50]. Such increases in hospitalization fees were made considering the additional need for care providers to treat severe COVID-19 patients who require more extensive management (including equipment such as an extracorporeal membrane oxygenation machines and ventilators) as well as the reduced efficiency of care due to personal protective equipment (PPE). There were no indications of additional increases in existing hospital fees in Germany, but support was provided for the costs involved in gaining access to hospital beds [15]. The amount of support provided per ICU bed equipped with negative-pressure facilities was equivalent to USD 56,818.18 (EUR 50,000) per bed.
The staff sub-domain involved support similar to that observed in the space sub-domain. This includes compensation for the burden placed on health care practitioners who care for confirmed patients receiving inpatient treatment. In Japan, support was also provided for outpatient services.
A detailed examination of benefits related to hospitalization fees revealed an increase in hospitalization fees in the space sub-domain, concurrent with inpatient management costs in the staff sub-domain [9]. First, the negative pressure isolation management fee in ICUs had doubled to USD 215.62 (KRW 255,940) while the negative pressure isolation management fee in ICU wards dedicated to severe COVID-19 patients had tripled to USD 431.25 (KRW 511,890). Furthermore, an infection prevention and control fee was newly established (USD 2.86, KRW 3,390) given that COVID-19 patients require isolation and additional efforts to prevent transmission to other patients. Similarly, an additional fee for emergency management was implemented in Japan [49]. Considering the potential additional treatments and tests needed to identify patient statistics as well as ordering additional drugs and ventilators in the process of caring for critically ill confirmed patients, fees had increased by up to five times. In Germany, compensation of USD 43.18 (EUR 38) was also provided for the increase in nursing work for treating confirmed patients [15].
Moreover, due to the difficulties in securing hospital beds in Korea, “residential treatment centers” were created for confirmed COVID-19 patients with mild symptoms for monitoring, diagnosing, and testing and for transferring worsening cases to nearby hospitals. Based on the type of service provided in each facility, costs were classified as I, II, or III and compensated accordingly [9]. Category I included support for patient consultations, monitoring, and chest X-rays through the provision of healthcare practitioners and X-ray equipment. Category II included the same services as under Category I (excluding X-rays), and Category III included greater benefits for patients admitted to one of the main residential treatment centers equipped with better medical facilities or those transferred to a residential treatment center from a medical institution as they required more intensive medical care than under Category I or II.
Among confirmed patients, those requiring specific care received relevant benefits. In Korea, compensations of USD 270.68 (KRW 321,300) were provided for treating dialysis patients [9] while, in Japan, compensations of USD 26.14 (JPY 2,980) were provided for outpatient dental treatment [51].
The stuff sub-domain involved compensations to alleviate the economic burden of PPE such as masks. Among the countries analyzed, compensation for PPE was provided in Korea and Germany. In Germany, compensation for PPE was increased from the initial amount of USD 56.82 (EUR 50) in April to USD 113.64 (EUR 100) in July [15]. Furthermore, compensation was also provided for PCR tests used to confirm COVID-19 infection. This benefit was applied in Korea, Germany, and the United States in February and in Japan in March, more quickly than benefits related to the treatment of confirmed patients [9, 52,53,54,55]. Furthermore, in February, the United States first approved a testing kit developed by the Centers for Disease Control and Prevention to confirm COVID-19 diagnoses and extended its insurance benefits to include the usage of such testing kits developed in the private sector to expand supply levels. In April, the insured value for testing kits increased from USD 51 to USD 100 [53, 54]. Germany also approved testing kits in February and introduced an insured value of USD 67.05 (EUR 59) [26].
The non-COVID domain mainly involved policy interventions in the staff sub-domain. No policy interventions were implemented for the space and stuff sub-domains other than the comprehensive benefits in Germany provided for the reduction in patients due to COVID-19. In Germany, an insurance fee of USD 409.09–863.64 (EURO 360–760) was applied to account for the reduction in patients resulting from postponed treatments or delays due to the treatment of COVID-19 patients [15].
While support in the COVID-19 domain was focused on inpatient services, support in the non-COVID domain usually involved support for outpatient services. In the staff sub-domain, all countries except Germany expanded benefits for virtual consultations. Telemedicine was implemented in Korea and Japan, where virtual consultations were previously not permitted, for a cost of USD 4.16 (KRW 4,940) and USD 18.77 (JPY 2,140), respectively [50]. In Korea, the respective fee could be claimed in addition to the basic consultation fee while, in Japan, USD 18.77 (JPY 2,140)—an amount lower than the previous initial consultation fee of USD 25.26 (JPY 2,880)—could be claimed. In the United States, where virtual consultations had already been available, only fees occurring in rural areas or areas with a shortage of healthcare practitioners were covered. Meanwhile, during the public health emergency period due to COVID-19, compensations were made eligible for a greater scope of services, locations, and service methods (e.g., video, telephone, online) [56]. Furthermore, in Korea, families of patients with a chronic disease requiring long-term prescriptions were granted permission for proxy access to prescriptions with an insurance fee of USD 4.96 (KRW 5,890), approximately 50% of the existing consultation fees.
Furthermore, to create a safe environment for non-COVID patients to receive treatment while preventing infections, compensation was also implemented for such services. In Korea, National Safe Hospitals and clinics dedicated to respiratory diseases, with segregated access, treatment, and care settings, were introduced to enable non-COVID patients to receive in-person treatments without the fear of infection, along with an infection prevention and control fee (USD 17.63, KRW 20,930). An infection prevention and control fee (USD 0.99, KRW 1,170) for implementing infection control protocols such as mask-wearing was also provided for patients in locked wards in mental and long-term care hospitals with many vulnerable elderly patients [9].
However, in Japan, compensations were offered for all outpatient or inpatient services, drug dispensing, and visiting nursing care without additional conditions [57]. Furthermore, for the testing of untested suspected COVID-19 patients, the infection prevention and control fee of USD 26.32 (JPY 3,000) was compensated [49]. Additional benefits included compensations for children under the age of 6 considering the higher likelihood of contact with healthcare practitioners [51].
Such policy support for health insurance was made possible through health insurance financing as well as national financial support. In Japan, the government budget regularly contributed toward health insurance financing as various support measures were modified or added [51, 58]. In Germany, the Hospital Relief Act was enacted in March 2020 to alleviate the financial support and administrative burden of medical institutions through the various aforementioned health insurance policies. Additional funding for this implementation was provided through taxes and contributions [59]. In the United States, in accordance with the CARES Act enacted in March 2020, matters related to the expansion of Medicare coverage and the like were stipulated along with an announcement that the funds for the changes would be sourced from the national disaster medical system [26].
Easing administrative regulations of health insurance
Aside from the additional financial compensation, regulations pertaining to health insurance administration procedures were relaxed to increase efficiency in the management of medical institutions (Table 3).
In Germany and the United States, the screening of medical expenses during a COVID-19 outbreak, or for COVID-19-related activities, was eased [59, 60]. Such measures were enforced in recognition that services were provided based on medical necessity without evaluating the adequacy of the provided medical service to alleviate the time and cost needed for the review process considering the situation’s urgency [59].
In addition to the easing of the review of medical expenses, the reimbursement period of health insurance claims was shortened in Korea and Germany [15, 61]. In Korea, payments were made in advance (90–100% of health insurance benefits for the same month of the previous year paid to the medical institution prior to settlement) or early (90% of the payment is made 10 days after the claim and before the completion of the evaluation). Through this process, the usual period of 22 days that it took medical institutions to receive the payment was reduced to 10 days.
Existing obligations to report staff or facility changes in institutions were also suspended. Although, in Korea, changes in human resource are linked to differential compensation payments and thus must be updated promptly, the duty to report was suspended. Additionally, contents of previous reports were applied in response to the frequent occurrence of unavoidable changes such as the isolation of healthcare practitioners after close contact, treatment of confirmed COVID-19 patients, or dispatch to other medical institutions [61]. In Japan, although a reduction in medical expenses is applied if the approved number of beds exceeds the number outlined under the Medical Act, the reduction was not applied for beds used to treat COVID-19 patients [50]. Furthermore, similar to Korea, reports on the changes in human resources due to a temporary surge in patients or the isolation of medical staff were suspended. Moreover, in the context of Korea, although DRG payment is underway for certain diseases or institutions, compensations of COVID-19 patients were based on fee-for-service payment to prevent the likelihood of under-compensation that can occur with bundled payments [9].
link